Distal Radius Fracture: A Comprehensive Overview
A distal radius fracture is a break in the radius bone at the end closest to the wrist. It is commonly referred to as a wrist fracture and may occur alone or in combination with injuries to the ulna or surrounding soft tissues. The most frequent mechanism is a fall onto an outstretched hand (FOOSH), where the wrist absorbs the impact force. This is particularly common during slips on ice or snow, sporting injuries, and everyday falls.
In younger individuals, fractures often result from high-energy trauma such as cycling accidents or contact sports. In older adults, especially those with osteoporosis, even low-energy falls can cause distal radius fractures.
The Bones of the Wrist
The radius is the larger of the two forearm bones and plays a critical role in wrist motion and load transfer. The distal radius articulates with the carpal bones to form the radiocarpal joint and with the ulna at the distal radioulnar joint (DRUJ), which allows forearm rotation.
Key anatomical features commonly involved in distal radius fractures include:
- Radial styloid
- Volar (palmar) surface
- Dorsal surface
- Distal radioulnar joint (DRUJ)
Disruption of these structures can alter wrist biomechanics and impair grip strength and range of motion.
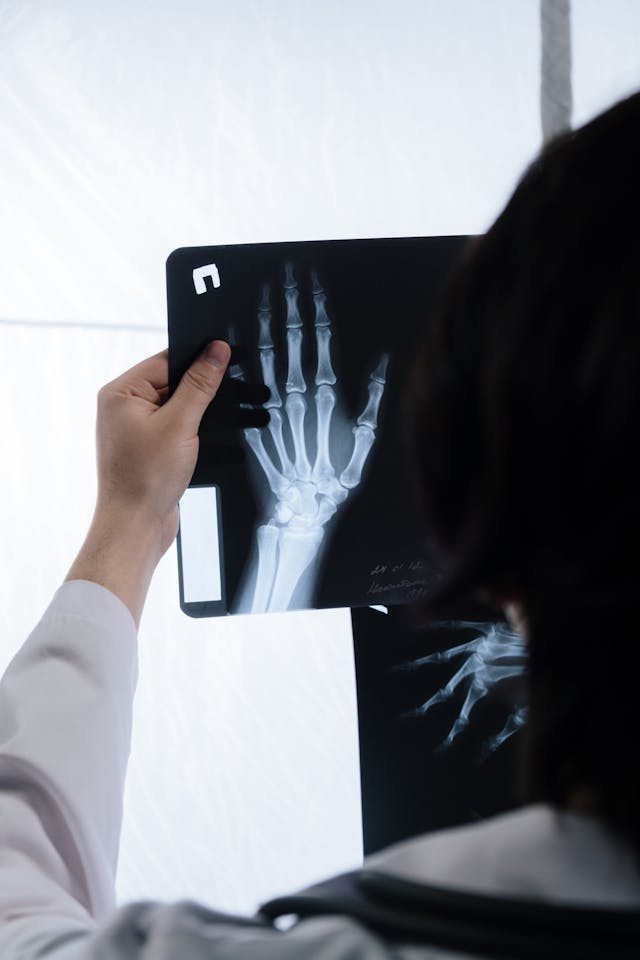
Symptoms / Clinical Presentation
Patients typically present with:
- Acute wrist pain
- Swelling and bruising
- Visible deformity (often described as a “dinner-fork” appearance)
- Reduced or absent wrist movement
- Tenderness on palpation
- Possible numbness or tingling due to nerve involvement in severe cases
Diagnosis is confirmed with plain radiographs, with CT scans occasionally used to assess complex intra-articular fractures.
Grades of Fracture from Mild to Severe
Distal radius fractures vary widely in severity and classification includes:
Mild (Stable, Non-displaced):
Minimal or no displacement
Extra-articular
Good inherent stability
Moderate (Displaced):
Angulation or shortening
May involve the joint surface
Reduction often required
Severe (Unstable or Comminuted):
Multiple fracture fragments
Intra-articular involvement
Associated ligament or DRUJ injury
Severity plays a key role in determining management and prognosis.
Conservative Management
Conservative treatment is appropriate for stable and minimally displaced fractures and may include:
Closed reduction
Immobilisation in a cast or splint for 4–6 weeks
Early finger movement and later Occupational Therapy
When alignment is maintained, conservative care produces good functional outcomes, particularly in low-demand patients.

Surgical Management
Surgery is considered for:
Unstable or significantly displaced fractures
Intra-articular fractures
Failure of conservative treatment
Surgical options include:
Open reduction and internal fixation (ORIF) with volar plates
Percutaneous pinning
External fixation
Evidence suggests surgery provides improved anatomical alignment and faster functional recovery in selected patients, although long-term outcomes may be similar to conservative care in elderly populations.
Outcomes / Expected Recovery
Bone healing typically occurs within 6–8 weeks, with gradual improvement in strength and motion over 3–6 months. Some patients experience residual stiffness or weakness for up to a year.
Outcomes depend on fracture severity, treatment method, patient age, bone quality, and adherence to rehabilitation.
References to Current Literature
Chung KC, et al. Treatment of distal radius fractures. J Hand Surg Am. Mulders MAM, et al. Operative vs non-operative treatment of distal radius fractures. JBJS. Silva Moreira A, Perugino M. Surgical vs conservative management systematic review. SIC Journal, 2023. BMJ Musculoskeletal Disorders (2023). Functional outcomes following distal radius fracture management.
